Blog

April 8, 2026
CMS Final Notice: Don’t panic, make a plan

Keith Anderson
Chief Executive Officer
Keith is the chief executive officer at Cozeva + Vatica.
The changes outlined in the CMS 2027 Final Notice have sparked a record number of comments across the industry. In my role as CEO of Cozeva + Vatica, I’ve heard similar questions and concerns from health plan leaders. The proposal to exclude unlinked chart record reviews, combined with a minimal rate increase and the ongoing impact of v28, has many plans justifiably scrambling.
As plans evaluate options to comply with the Final Notice and prepare for future changes, common themes I hear are:
- Plans understand the advantages of having providers support risk adjustment prospectively at the point of care, as opposed to retrospective reviews and home visits.
- Plans engage providers in risk adjustment now, but often with minimum success. PCPs are overwhelmed with payer-specific asks and unique incentive models that are difficult to track.
- Plans deploy overlapping risk adjustment efforts on the same member, compounding expenses and making it difficult to understand the distinct value of each initiative.
- Plans are steadily improving the percentage of linked HCCs, but not enough to avoid loss of value outlined in the Final Notice.
What advice have I offered to these health plan leaders?
- First, a swift focus and potential investment in linking diagnosis to encounters should be a priority.
- Secondly, recognize that this is one of several changes expected as CMS encourages plans to link member diagnoses to the actual treatment of care. Thus, the best and most durable method for risk adjustment in the future is a provider-led solution.
- As it relates to activating your provider network – don’t go at it alone. Keep in mind, the average provider contracts with eight Medicare Advantage plans. It is unlikely payers can get provider adoption for their membership alone. Partner with companies like Vatica that aggregate payers into a single process and consistent workflow to increase provider activation.
- Lastly, after you’ve activated your provider network, eliminate overlapping solutions. Providers documenting at the point of care is the gold standard of risk adjustment. After that is accomplished, save yourself the expense, and eliminate other solutions.
To sum it up, the new operating model for risk adjustment requires the capability to:
- Produce encounter-linked documentation.
- Integrate diagnosis coding into the PCP workflow.
- Reduce abrasion for provider networks through process consistency.
- Ensure PCP attestation.
- Produce a better patient experience and better outcomes.
Plans that move early will not only protect revenue — they will build a more durable, provider-aligned model for the future of risk adjustment. If you need assitance, we can help. Vatica and our new merger partner, Cozeva, we are trusted by 30 health plans and 120,000 providers. Contact us today to get started.
Case study
Relieve the burden of coding and documentation
Provider members of the Kentucky Primary Care Clinically Integrated Network found support in the Vatica program at no cost. Vatica relieved the burden of coding and documentation while generating additional health plan compensation. Read our case study for the noteworthy results.
Relieve the burden of coding and documentation with Vatica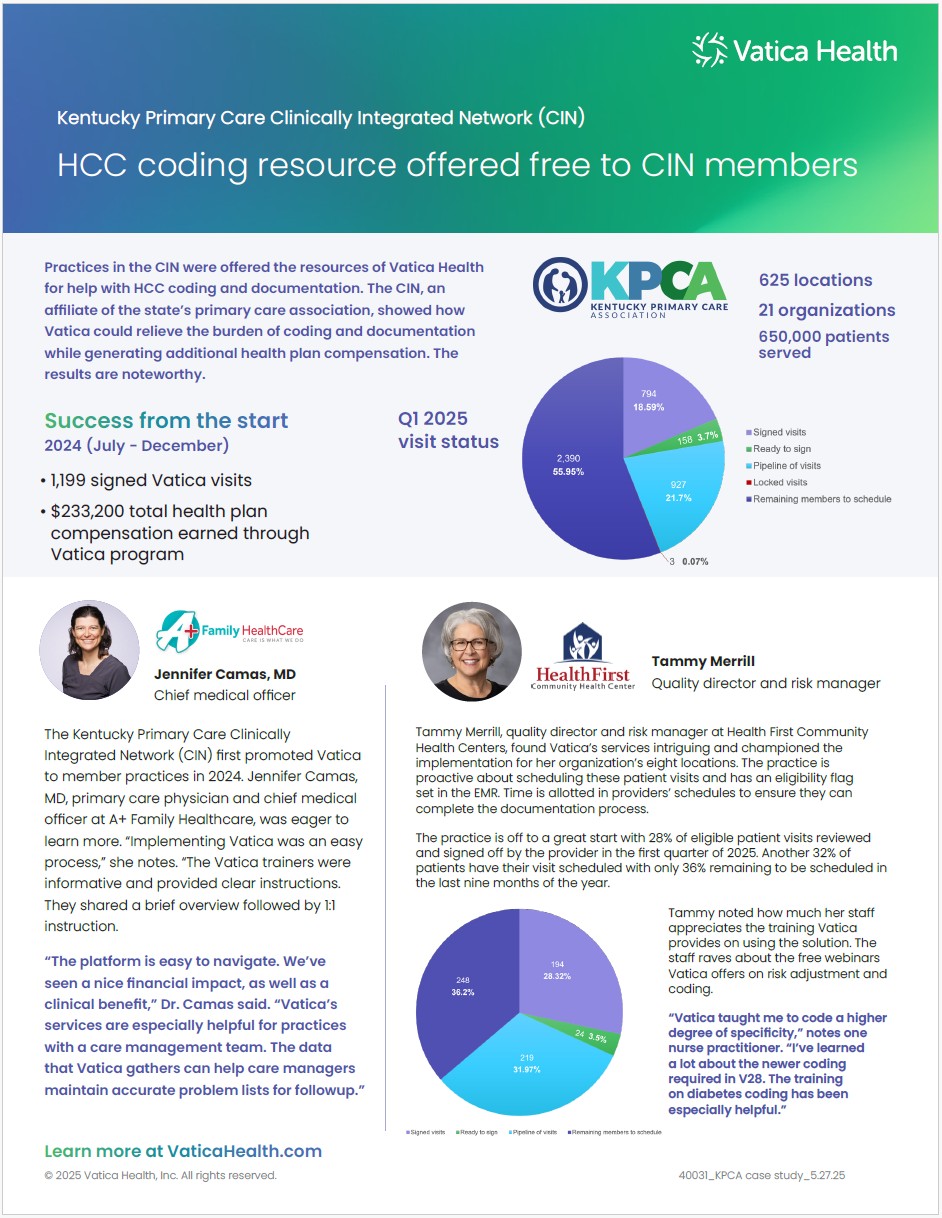
Resources
Read our latest thoughts
on healthcare

Subscribe to Vatica Voice
Get our latest news and insights delivered directly to you.
Adjust your approach to risk adjustment
Talk to one of our risk adjustment experts today to see how we can help you deliver better performance and stronger compliance while closing gaps in care.