CMS 2027 Final Notice

What you need to know
CMS released the 2027 Final Notice on April 6, 2026. Many of the key changes proposed in the Advance Notice appear in the Final Notice, with a few key exceptions.
Key provisions
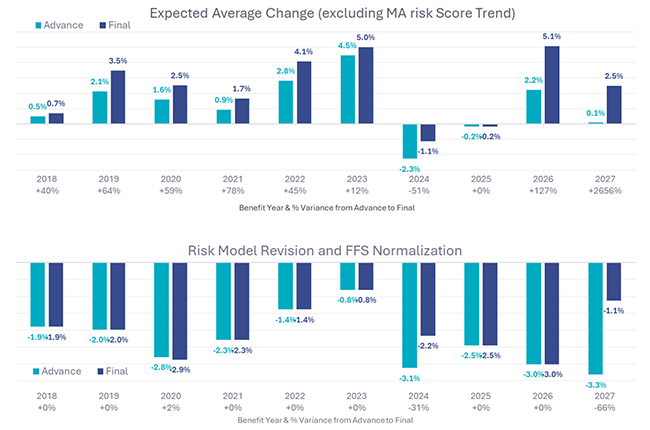
- Payment: Overall expected average change to Medicare Advantage revenue has been modified from the proposed +0.09% to +2.48%. This is due to eliminating the proposed v28 Risk Model Revision. Impact revised from -3.32% to -1.12% to reflect normalization only.
- Unlinked chart record reviews: Starting with 2026 dates of service, audio-only and unlinked chart review records (CRRs) will be excluded from MA risk adjustment, as described in the Advance Notice.One notable adjustment: CMS “is finalizing an exception for unlinked CRRs for beneficiaries who switch from one MA organization to another.” This is a practical change: a patient’s new MA plan is not likely to have access to ICNs associated with original EDR (claims) submissions from a previous MA plan.
- V28 model refresh: Not moving forward.
- A recalibration of the RxHCC model using 2023/2024 diagnoses, as described in the Advance Notice, will be upheld.

Putting the changes into context
- The 2027 Final Rule total expected change to MA revenue (+2.5%) is in line with the prior nine-year average (+2.4%).
- However, the resulting revision from the Advance Notice to Final Rate Notice (+239 basis points) is second only to 2026 (+283 basis points).
- For comparison, the average revision from 2018 to 2025 was +77 basis points.
- 2026 revision was primarily driven by a 52% increase to growth rate, whereas the 2027 revision is driven by CMS’s decision not to implement the proposed v28 model revision.
Implications for the future
While plans may breathe a sigh of relief from the better-than-proposed revenue impact, CMS is sending a clear message. While the agency wants to help address health plans’ challenges in the short term, additional changes are coming to support long-term stability in the MA program.
Chris Klomp, director of Medicare, said that officials expect plans “to do their best work in controlling costs.” We believe that the original rate of 0.09% in the Advance Notice, boosted when CMS removed recalibration from the equation, is a good indicator for 2028 and beyond.
The removal of 11 Star measures and exclusion of unlinked CRRs also signal CMS’ focus on cost containment, as well as improving outcomes for patients. While the Star measures removed are considered to have minimal impact–“checking the box” for plans–CMS kept a diabetes measure that proponents argued resulted in meaningful clinical improvements.
Likewise, the exclusion of unlinked CRRs is not the last change CMS will make to eliminate concerns about upcoding and tie risk adjustment to care delivery. It’s likely home visits will be next for additional regulation or elimination from risk adjustment processes.
The sentiment for physician-led risk adjustment is bi-partisan and will continue for the foreseeable future. Given this environment, we don’t recommend that health plans address policy updates one at a time. Rather, plans should anticipate the direction of risk adjustment reform and implement comprehensive, future-ready strategies.
For a look at future CMS policy predicated on historical data, watch our webinar with Capstone.

Where do you go from here?
For our customers:
- We are updating platforms and analytics to reflect the 2023/2025 RxHCC model revision.
- We will continue monitoring MA CRR linkage rates and patterns for our MA clients, collaborating to increase the rate.
Not a customer but want to learn more?
PCPs coding and documenting at the point of care is the gold standard of risk adjustment. The Cozeva + Vatica solution is PCP-focused, used at the point of care and payer-agnostic.
Implement the gold standard in your organization. Click below to request a consultation.

Want more detail?
- CMS Fact Sheet
- CMS Final Rule
- CMS Announcement & Documents Inventory
- Our CEO’s advice on how to develop your plan

Adjust your approach to risk adjustment
Talk to one of our risk adjustment experts today to see how we can help you deliver better performance and stronger compliance while closing gaps in care.